
Protecting the Herd
It’s called “herd immunity,” or “community immunity,” and has been making headlines and into everyday conversation among everyday people. As a society we had become so reliant upon it that unless you were among the vulnerable you didn’t think much about it. For most people it meant no more worrying about measles or polio. For those with underlying conditions it was a shield from a potential life-or-death situation.
Germs from viruses can make their way quickly through a community. Some are fairly benign as in the case of the common cold. But others can pose a threat to otherwise healthy people, and are a serious cause for concern for those with underlying conditions. Illnesses such as cancer, diabetes, hypertension, autoimmune diseases, or COPD make it harder for a body’s immune system to fight off infection. Treatment for those illnesses can leave a person immune-compromised, leaving them doubly vulnerable.
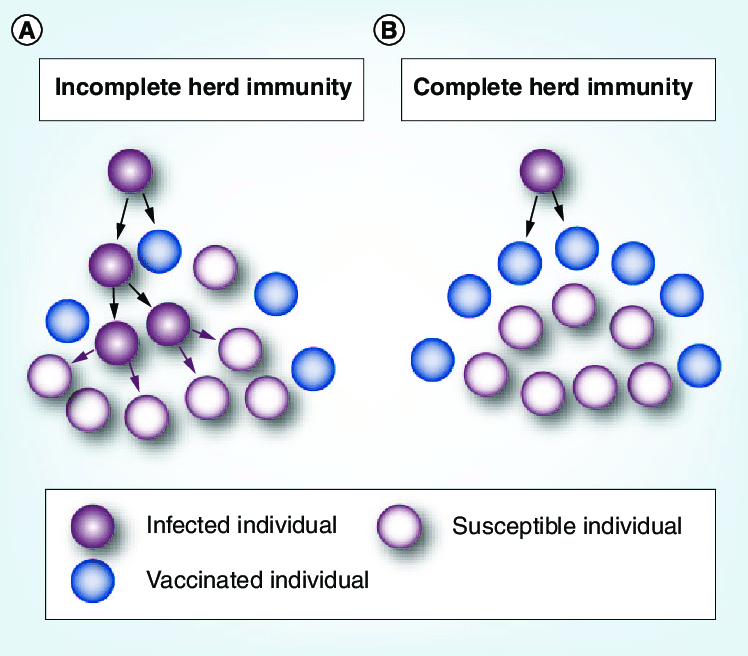
A term created by veterinarians, “herd immunity” is defined as “the indirect protection for a contagious infectious disease that happens when a population is immune either through vaccination or immunity developed through previous infection.” Meaning that even if a person can’t be vaccinated, they are protected because those around them are immune, therefore not passing along disease. Eventually, once herd immunity is established, diseases can become rare or eradicated, as in the case of smallpox.
Prior to the middle of the 20th century, thousands of people died from measles, mumps, polio, whooping cough and rubella. Natural herd immunity, achieved through infection, was challenging to induce without a lot of serious illness and death. Once vaccines were developed we saw those diseases nearly eliminated. Widespread adoption of vaccines protected individuals and the community at large. In recent years people choosing not to vaccinate, “anti-vaxers,” have garnered attention as measles and whooping cough and other diseases have crept their way back into our population, leaving the vulnerable exposed to old threats.
But COVID-19 has brought the discussion of vaccines and herd immunity to the forefront, ringing the bell and giving us a harsh reminder of why they are so vital. This novel virus has halted work, altered lifestyles and damaged economies worldwide. Here in the U.S. it’s responsible for the loss of tens of thousands of lives in a matter of weeks, and confounded the scientists we assumed could protect us from disease. Some believe that relying the development of natural herd immunity is the way forward, but scientists warn that millions more people will be lost if that’s the path.
Developing herd immunity is challenging. Scientists at the NIH believe that this particular virus will need 70% or higher population immunity to develop herd immunity and that it won’t be reached until 2021 at the earliest. We can all live in hope that herd immunity will magically develop, but without widespread adoption to vaccines we may not achieve it without suffering devastating loss of life. A vaccine is critical to achieving it and to saving lives.
Hope Trust serves clients throughout the United States.

